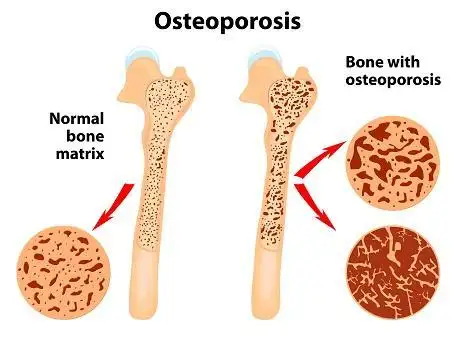
Osteoporosis is commonly seen in large numbers nowadays. Post menopausal women and men of age 70 years and above are at an increased risk for this condition. Bone Mineral Density (BMD) is the test which measures the amount of minerals such as calcium in your bones. It is done using X-ray and Computed Tomography (CT) scan. This information is then used to estimate the strength of your bones.
Most common fractures associated with post menopausal osteoporosis occur at the hip, spine and wrist. The first two are of prime concern as hip fractures usually require major surgery, and involve joint replacement and loss of independence. Mortality rates are also high due to surgery at old age. Spine fracture can lead to intense back pain and deformity. Post menopausal osteoporosis is thus considered a serious public health concern due to its high prevalence world wide.
Existing therapies for osteoporosis use anabolic and anti-resorptive agents. Biphosphates are anti-resorptive agents that slow down the bone breakdown process. They do not show a marked increase in BMD and they do not have any action in restoring the bone structure. Anabolic agents like Teriparatide which are currently used in market have a drawback. The injections are required to be taken daily and carry chances of a bone cancer called osteosarcoma.
A path breaking new research suggests the use of Romosozumab, an anabolic agent, can transiently stimulate bone formation and chronically suppress bone resorption. Sclerostin is an osteocyte-secreted glycoprotein which impedes new bone proliferation and activity; treatment with romosozumab, an anti-sclerostin antibody, is therefore expected to enhance bone formation. In the research it was found that Romosozumab can significantly improve bone mineral density (BMD) at the lumbar spine, total hip and femoral neck in postmenopausal women with low BMD. Importantly, when given at a dose of 210 mg monthly, Romosozumab increased BMD to a greater extent than either Alendronate or Teriparatide.
REFERENCES:
- Elizabeth Hofheinz, M.P.H., M.Ed. Study- ROMOSOZUMAB significantly increases BMD, Orthopedics This Week, Fri, January 10th, 2014. www.ryortho.com
- www.medscape.com
Related Posts
Cigarettes May Inhibit Inflammation Treatments
Axial spondyloarthritis, also known as AxSpa, is a chronic…